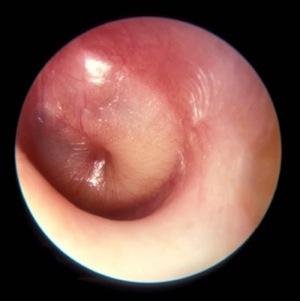
A view of the tympanic membrane showing acute otitis media, also known as a middle ear infection. New pediatric guidelines urge doctors to verify the distinct bulge when diagnosing an ear infection, to curb the overuse of antibiotics. (File/CC/Sharing in Health)
Middle ear infections are one of the most common reasons kids see doctors and the leading reason kids get antibiotics. But about 70 percent of children get better on their own within two or three days, and about 80 percent are better within a week to 10 days, according to Richard Rosenfeld of the State University of New York Downstate Medical Center, who helped write the new guidelines.
The 2013 guidelines, published in the March issue of the journal Pediatrics, are for uncomplicated acute otitis media at ages 6 months to 12 years in otherwise healthy children without other factors such as immune deficiencies or cochlear implants.
Rosenfeld noted that there are downsides to using antibiotics when they're not necessary. Aside from contributing to the rise of antibiotic-resistant "superbugs" that are tough to cure, they can cause upset stomachs, allergic reactions and other side effects. "The bacteria that do survive the antibiotic get tough, and next time you get an ear infection or any other type of infection, they're harder to manage," Rosenfeld says.
"Parents, if their child is up all night screaming and tugging the ear, they want something to make the child feel better," Rosenfeld says. "You don't have to freak out as a parent. [Ear infections] tend to go away on their own quite often with just some pain medicine."
The new guidelines also provide stricter diagnostic rules. "There are dozens of reasons an ear can hurt," Rosenfeld says. "In this guideline we say, 'Listen, if you're not sure of the diagnosis, don't even think about giving an antibiotic. Please, don't even think about it.' "
The only way to know for sure is to take a close look at the eardrum and see if it is clearly bulging. But even kids who really do have ear infections don't necessarily need antibiotics. The guidelines say doctors have the option of just watching kids who don't have intense pain, a high fever or other symptoms of a severe infection.
But children aged 6 months to 2 years who have infections in both ears or any child who has severe pain for several days and a fever of at least 102.2 degrees should definitely receive antibiotics. Any child who has a ruptured eardrum should also get antibiotics, according to the guidelines. "If you have a severe infection, no point discussing it further. Those children are going to get antibiotics. And the reason is they'll get the most benefit," Rosenfeld says.