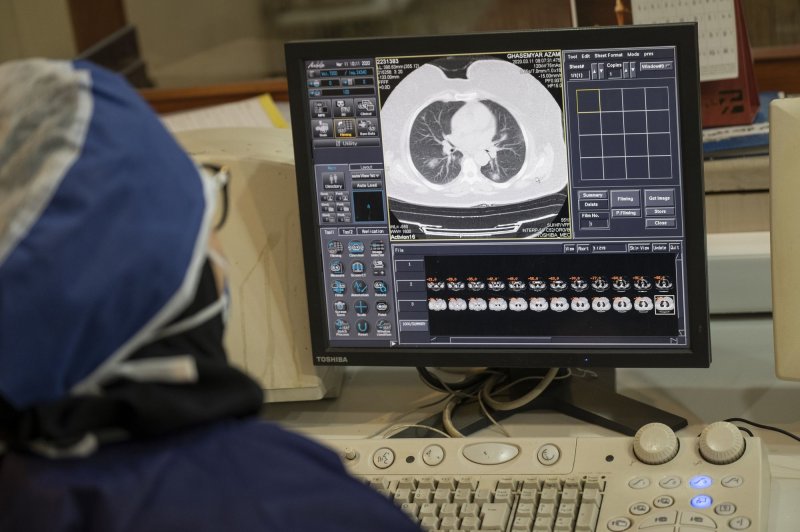
1 of 2 | Iranian medical personnel, wearing protective gear, check a scanned image of the lungs of a patient at a CT scan section of the Rassolakram hospital in western Tehran on March 11. Photo by Morteza Nikoubazl/UPI |
License Photo
March 26 (UPI) -- The COVID-19 pandemic started in Wuhan, China, as a cluster of unusually severe pneumonia cases of unknown cause. Now that the disease has spread globally, the lungs continue to bear the brunt of the infection in humans -- just as they do with conventional pneumonia.
A small study published recently in the journal Academic Radiology found that the new coronavirus impacted both lungs in nearly 80 percent of cases, with the vast majority showing significant injury or inflammation on computed tomography, or CT, scans.
"The virus that causes COVID-19 -- SARS-CoV-2, or severe acute respiratory syndrome coronavirus -- infects the cells that line the respiratory tract from the nose down into the lungs, where it causes cells to die and creates an immune reaction," Dr. Ben Singer, a pulmonary and critical care specialist at Northwestern Memorial Hospital, told UPI.
"That immune reaction helps to clear the virus, but can also cause damage to the lungs as well," Singer said.
Although the majority of people infected with COVID-19 either have no symptoms at all or feel like they have an upper respiratory tract infection -- a low-grade fever, cough, sinus congestion and headache or fatigue -- some may progress to what feels like a severe case of the flu, Singer said.
Researchers in Wuhan noted in a study published by The Lancet that this is how more than 60 percent of those infected experience the virus.
As many as 6 percent of people with the coronavirus develop pneumonia, an infection that impacts the lower respiratory tract -- the region below the larynx, according to an analysis published in late February by the New England Journal of Medicine.
Lower respiratory tract infections like pneumonia often result in serious illness because they can affect the ability to breathe, noted Dr. Raju Reddy, an assistant professor in the Division of Pulmonary, Critical Care and Sleep Medicine at University of Florida Health.
"People may have cough, sputum and shortness of breath," Reddy told UPI. "COVID-19 causes acute lung injury, which is characterized by air spaces getting filled with fluid, protein and cells. It is similar to other viral pneumonias in the end results -- inability for the lung to adequately oxygenate the blood."
The type of pneumonia associated with COVID-19 has been described as an infection that affects the air passages that move air between the lungs and the outside world.
With this infection, the lining of the air passages become inflamed and irritate nerves in the lining of the airway, Singer said. As the infection progresses, fluid can accumulate in the air passages and the air sacs at the bottom of the lungs, before spreading to the rest of the lungs.
It's this tendency to affect the entire lungs that makes pneumonia caused by the new coronavirus so unique -- and severe. Lungs filled with fluid are unable to send sufficient oxygen to the bloodstream. As a result, the body is less able to take on oxygen and get rid of carbon dioxide.
While some types of pneumonia are caused by a bacterial infection, and are thus treatable with antibiotics, this isn't true for all of them.
"Although most people do not realize it, most pneumonias are actually caused by viruses, including influenza," Singer said. "COVID-19 appears to cause severe pneumonia in a greater fraction of people than influenza, and it also spreads more easily."
At this point, there is no cure for the pneumonia associated with COVID-19, so doctors are focusing on providing "supportive care," Reddy said. This involves the use of ventilators to help the lungs maintain high oxygen levels until the infection resolves and the organs are able to function normally on their own.
This is the reason for concern over shortages of these machines at many U.S. hospitals.
"We provide supplemental oxygen by various methods and wait for the body to recover," Reddy said.
Roughly 1 percent to 2 percent of COVID-19 patients fail to recover, and researchers say those who do still might be at risk for developing secondary infections. They might be treated with antiviral drugs or antibiotics to blunt the impact.
"Fortunately, most cases of COVID-19 are mild and can be managed at home like one would care for a bad cold," Singer said. "When patients become sick enough to need the intensive care unit, they often require life support with a mechanical ventilator and other measures to support their bodies while the virus runs its course.
"We are interested in a number of medications that target either the virus itself or the immune reaction to the virus. These medications are best given in the context of a clinical trial."
A health worker with the Israeli national emergency service, Magen David Adam, wears protective gear while taking swabs to test for COVID-19 at a drive-through testing center in East Jerusalem on August 26. Photo by Debbie Hill/UPI |
License Photo