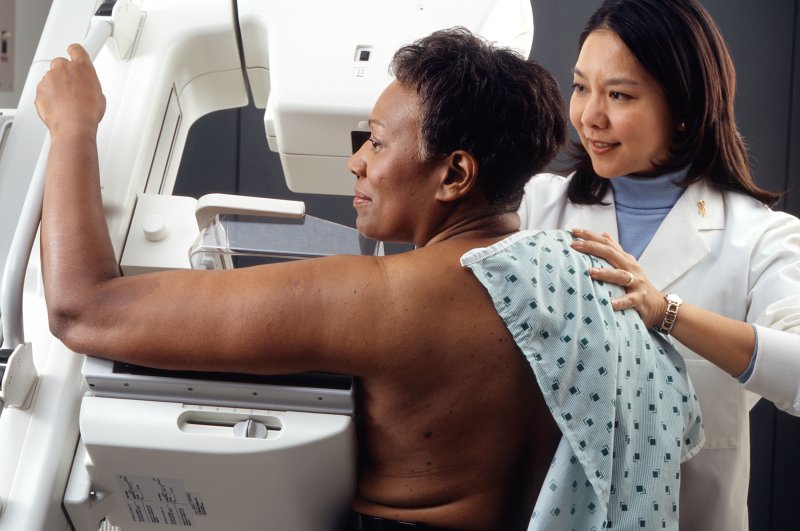
A technician positions a woman at an imaging machine to receive a mammogram. Photo by Rhoda Baer/Wikimedia Commons
March 23 (UPI) -- Private health insurers spend more than $2 billion a year to screen women in their 40s for breast cancer, though fewer than half those eligible undergo mammograms, a new study shows.
In results published Monday by JAMA Internal Medicine, researchers noted that just over 41 percent of women between age 40 and 49 who had private insurance had a mammogram in 2017. The mean per person cost among these women was $353, according to researchers.
"Breast cancer screening is associated with high costs," study co-author Natalia Kunst, a research fellow at the Yale School of Medicine and Public Health and a doctoral candidate in health decision science at the University of Oslo in Norway, told UPI.
"These substantial costs are borne despite the fact that health outcomes associated with breast cancer screening in this population remain uncertain and there is inconsistency between professional society guidelines for screening women" in this age group, she added.
Indeed, the lack of consensus regarding the value of routine mammograms for women in their 40s has resulted in significant confusion.
Currently, the U.S. Preventive Services Task Force recommends that women begin breast cancer screening at age 50, while the American Cancer Society recommends women have their first mammogram at 45.
Most private insurance companies in the United States reimburse patients in their 40s for the costs of a mammography, despite concerns over lack of accuracy and exposure to low-dose radiation associated with the procedure.
For their study, Kunst and her colleagues reviewed data on more than 2.2 million women from the Blue Cross Blue Shield Axis, a large commercial claims database, focusing on women 40 to 49 years old who were eligible to receive screening mammography in 2017.
Of the women included in the analysis, just over 930,000 were screened in 2017, with 543,380, or 24.1 percent, undergoing 2-dimensional mammography. Of this latter group, 387,146, or 17.2 percent, had the procedure with digital breast tomosynthesis, or DBT.
Among the women who had a screening mammography, 137,764, or 15 percent, were recalled for diagnostic evaluation and 20,229, or just over 2 percent, were referred for other diagnostic tests.
The authors found that the main contributor to the overall cost of screening was the mammography itself -- this represented $249 of the $353 mean total per person cost -- followed by recall -- $56 -- and other diagnostic tests -- $45.
In all, after extrapolating these costs to the U.S. population with private insurance, the total national cost of screening women in their 40s was $2.13 billion per year, most of which was accounted for by the initial screening mammography.
"Our findings indicate the importance of determining if the benefits of screening women in their 40s outweigh the potential harms," Kunst said. "We hope that a better understanding of real-world utilization and costs of breast cancer screening in this population will enable healthcare policymakers to perform more accurate decisions about breast cancer screening women in their 40s."