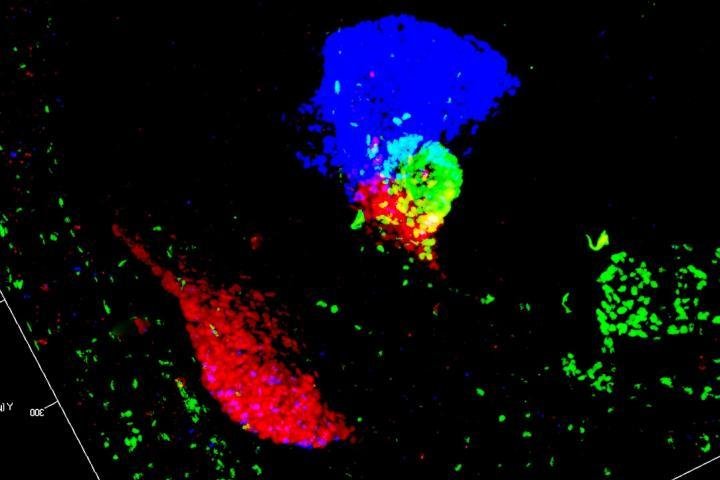
Researchers have reprogrammed liver cells from mice into pancreatic cells, which could lead to a treatment for type 1 diabetes. Pictured, a 3D map of liver and pancreatic buds in a mouse embryo. Cells of the pancreas are marked in red and green, while liver cells appear in blue. Photo by Francesca Spagnoli/MDC
Feb. 13 (UPI) -- Researchers in Germany have successfully reprogrammed liver cells into pancreas cells for the first time outside the body in mice, which could lead to a new treatment for type 1 diabetes patients.
A team from the Max Delbruck Center for Molecular Medicine in the Helmholtz Association, or MDC, put liver cells into an "identity crisis" by reprogramming them to be in a less specialized state and then stimulate their development into pancreatic cells by altering the activity of a single gene.
In type 1 diabetes, a person's immune system destroys pancreatic islet cells responsible for the production of insulin resulting in a rise in blood glucose and insulin dependence through injections.
The gene TGIF2 is found in pancreatic tissue but not in the liver, and plays a vital role in the process of reprogramming liver cells into pancreatic cells.
Researchers tested how liver cells in mice act when they are given additional copies of the TGIF2 gene and found that the cells first lose their liver properties then acquire properties of the pancreas.
The glucose levels of the mice then improved showing that the cells were replacing the functions of the lost islet cells.
The team, led by Francesca Spagnoli, Ph.D., MDC group leader and study author, could lead to new treatments for type 1 diabetes by growing new pancreatic cells outside of the body.
"There are differences between mice and humans, which we still have to overcome," Spagnoli said in a press release. "But we are well on the path to developing a 'proof of concept' for future therapies."
The study was published in Nature Communications.