LOS ANGELES, Feb. 18 (UPI) -- A clot-busting drug used for heart attacks and non-bleeding strokes can be used to reduce post-stroke disability and mortality in patients with a type of bleeding stroke, researchers found in a recent clinical trial.
The drug Alteplase, a tissue plasminogen activator, or tPA, cleared blood that pooled in the brains of people with intraventricular hemorrhage, reducing death rates by 10 percent and nearly doubled the likelihood of a more functional recovery, researchers reported at the 2016 International Stroke Conference.
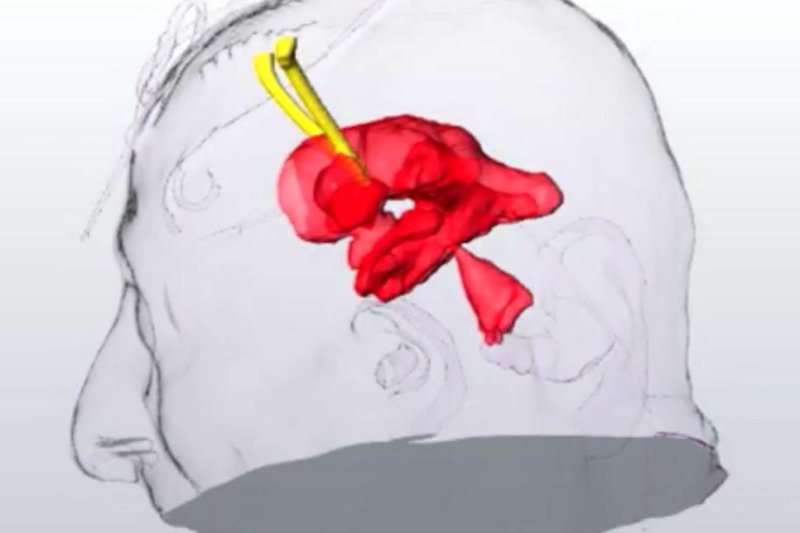
Intraventricular hemorrhage is a form of stroke characterized by blood pooling and clotting in the brain's ventricles, which normally hold cerebrospinal fluid. Intraventricular hemorrhage accounts for just 15 percent of all strokes, but they make up 40 percent of stroke deaths.
Between 60 and 80 percent of patients do not survive intraventricular hemorrhage, and 90 percent of those who survive recover very little of their former functionality.
"For many patients, this approach can significantly reduce disability after a stroke, and can be the difference between going home instead of going to a nursing home," Dr. Issam Awad, a professor of surgery at the University of Chicago, said in a press release.
For the study, researchers enrolled 500 patients around the world with intraventricular hemorrhage, treating them with either tPA or saline through a brain catheter. The participants were followed for five years after treatment, from 2009 to 2015.
Death rates among patients given tPA went down by 10 percent, and were one-third lower than the saline group's death rate.
Eighteen percent more patients with larger clots -- greater than 20 mL of pooled blood -- who got tPA had "good outcomes" than those who received saline, and 79.8 percent of patients given tPA had 80 percent clot removal. Patients with 90 percent of their clots removed had more than double the chance of "good" outcome, the researchers reported.
"When we entered into the trial, we knew very little about how this therapy ought to be used, in whom it should be used, and whether it was safe," Awad said. "We now have clear data on how best to implement the procedure, and for at least a group of patients, we know it can nearly double the likelihood of a favorable outcome."